Evolution of an Algorithm: Lessons from the Kidney Allocation System
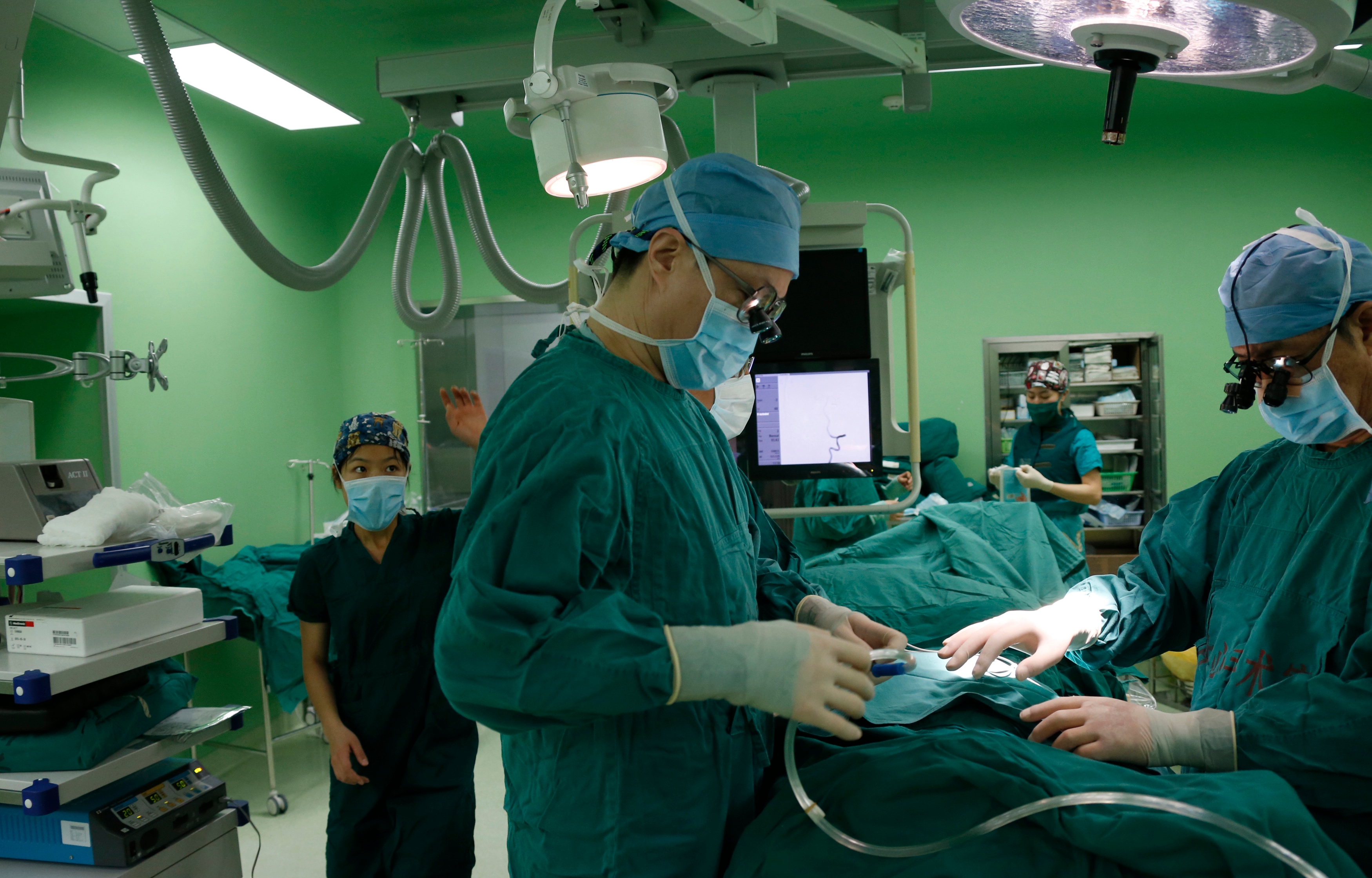
Public input and transparency were key to overhauling this critical decision-making algorithm.
Who should get a kidney first?
It’s a critical, life-or-death question, with about 115,000 hopeful kidney transplant recipients in the U.S. currently. And it’s ruled by an algorithm.
The recent overhaul of the U.S. kidney allocation system offers a valuable look at the challenge of creating an AI-based decision-making algorithm for organ allocations, says David Robinson, visiting scientist at Cornell University’s AI Policy and Practice Initiative. Robinson, cofounder and managing director of Upturn, a nonprofit promoting justice in digital technology, spoke during a Stanford Institute for Human-Centered Artificial Intelligence weekly seminar about his research into the system’s redesign as part of his broader effort to write a book on AI-driven decision making.
“People are judged by these algorithm-based systems but often can’t understand them or influence their design and values choices,” he says. “And policymakers lack expertise and confidence to ask key questions about algorithms.”
Here he explains what he learned from studying medical literature, federal statues, and allocation policy documents, as well as interviewing 10 experts including the surgeon who chaired the committee developing the underlying algorithm.
Governance of Transplants
The U.S. Congress passed the National Organ Transplant Act (NOTA) in 1984, designating transplantable organs as national resources that can’t be sold. The legislation directed the government to create a system to match organs with recipients. The United Network for Organ Sharing (UNOS), the nonprofit set up to oversee the program, maintains the digital system that prioritizes recipients when a kidney becomes available.
But the original system missed clear opportunities to maximize the long-term value of an available kidney, instead awarding an organ from a young donor to an older recipient with low life expectancy, or matching an organ from an elderly donor with a young recipient, which often resulted in the need for a future transplant.
“Such waste was a moral and legal problem,” Robinson says. The situation prompted a national mandate to improve the transplant decision system.
Overhauling the System
Starting in 2003, UNOS led the process to rewrite the kidney transplant algorithm, which included multiple public debates.
Early revision focused mostly on maximizing the number of life years recipients gained from the transplant, or LYFT. But the discussion also considered factors such as equity based on race, age, and other factors. For example, a 2008 proposal would have maximized LYFT by prioritizing younger recipients across the board, but this disadvantaged older recipients.
A subsequent approach – known as the “20/80 Proposal” – matched organs to recipients based primarily on longevity: The youngest 20% of kidneys would go to the youngest 20% of recipients; the remaining 80% were assigned based on age-matching (donor and recipient no more than 15 years apart). This would have improved older applicants’ access, but the government argued the proposal violated the Age Discrimination Act by using age so explicitly for decisions in programs receiving federal funds.
Public input helped support this point. For example, a patient with polycystic kidney disease argued that prioritizing younger recipients penalized that patient for prolonging kidney life through healthy habits, placing them lower on the priority list as they aged.
The core kidney allocation system in place today was unveiled in late 2014. It abandoned age-matching for the youngest fifth of organs, basing it on waiting time instead, while applying age-matching to the oldest 20%.
“You might think that’s where the story ends,” Robinson says. But subsequent developments have refined the algorithm further.
The Problem of Geography
In 2017, New York resident Miriam Holman, who urgently needed a lung transplant, sued UNOS over disparities in geographic access, arguing that “donation service territories” were too arbitrary – for example, if a lung had become available just over the state border in New Jersey, it would have gone to a resident of that state, even if that person’s need was less severe than hers.
Holman’s argument highlighted geography as a major issue in organ allocation: Wait times can vary up to 20 times between territories; wealthy patients can join multiple transplant center waitlists and engage in domestic “transplant tourism” by undergoing procedures in centers far from their homes. While some amount of localism is inevitable due to logistics, these factors motivated many centers to maintain the status quo.
UNOS recognized the current system was flawed and revamped geographic boundaries to be the radius around each donor hospital, rather than fixed state-based lines.
Four Takeaways
The evolution of the kidney transplant algorithm offers multiple lessons that apply to any AI-based decision-making system impacting human lives. Robinson suggests four key ones:
Public input is critical but constrained. Promoting public input into the kidney transplant algorithm yielded better consensus on an equitable process, shaping stakeholder opinion. But legal and political authorities will bound the process, as happened for the longevity-driven model.
Seek out the experts. Access to voluminous information and documentation isn’t enough for meaningful participation and understanding, due to the complexity of such algorithm-based decision-making processes. Expert input from those involved in the process is deeply valuable. “Just a few minutes of conversation with those in the know changed my perspective,” Robinson says. “Lived experience is critical.”
Design drives attention. An algorithm’s design will sharpen focus on some issues while obscuring others. In the kidney allocation discussion, debates over equity took precedence while fewer people paid attention to arbitrary boundaries between donation service areas.
It’s an ongoing process. An algorithm’s performance must be publicly audited and analyzed, with annual reports, to create a common point of reference and evolve the system.
“It’s tempting to believe the software controls the moral stakes of an algorithm,” Robinson says in conclusion. “But the social surroundings are critical, and there needs to be a process for values to come in from outside the engineering team. There are lots of ongoing efforts to make algorithms more accountable, like disclosure of source code. It’s all evolving.”
Watch the full video of the seminar, below, or sign up for our email newsletter to learn about upcoming events.



