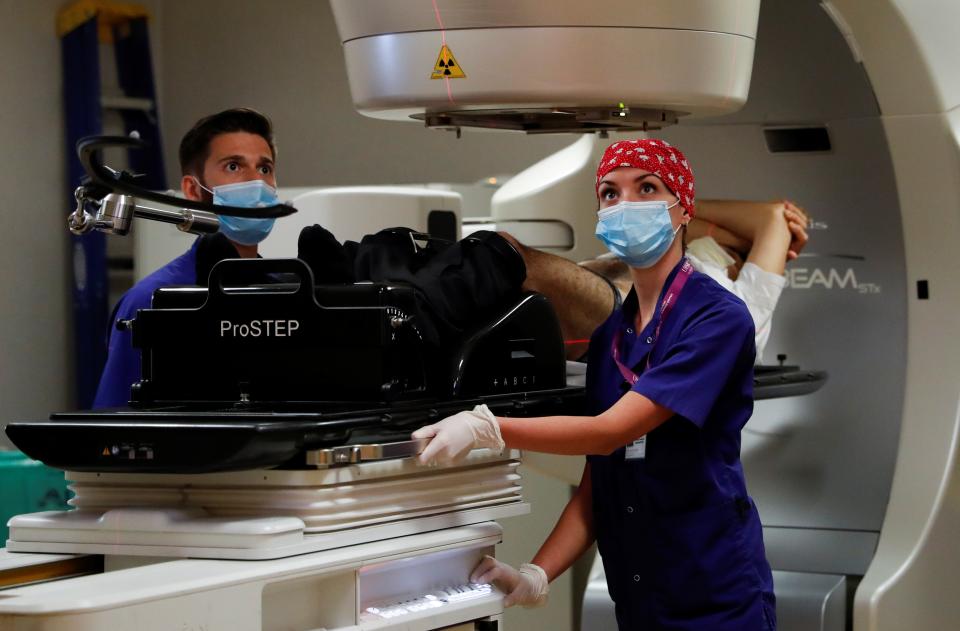
Medical staff members perform a stereotactic radiotherapy treatment on a patient. AI could help doctors better identify cancers and target the best treatment for that particular subtype. | Yara Nardi
Great strides have been made in recent years combining artificial intelligence and medical imaging to improve cancer diagnosis. Now a research team led by Stanford and including researchers from Texas, England, and Japan are using AI to help oncologists improve treatment for their patients.
“When most people think of radiology, they think of CT and MRI scanners finding the disease, but oncologists are often more interested in treatments for their patients,” said Ruijiang Li, associate professor in radiation oncology and a member of the Stanford Institute for Human-Centered Artificial Intelligence (HAI).
“We’ve used AI to help identify the subtype of cancer a patient may have and to target precision medicines that are best suited to their subtype,” explained Li, who is senior author of a paper describing a new approach to cancer treatment appearing in the journal Nature Machine Intelligence. Their study shows that specific cancer tumor structures respond better to specific treatment regimens, but they also then matched treatment to subtype to improve prognosis for patients with the given subtype.
Read the study: Radiological Tumour Classification Across Imaging Modality and Histology
Seeking Out the Patterns
Li says that even among specific types of cancer, like lung or breast cancer, not all tumors are the same. There are different subtypes that often respond to treatment differently. What works for one patient may not work for another.
To better understand how these subtypes respond to various treatments, Li and colleagues trained their AI algorithms on an existing international database of 1,682 cancer patients, each of whom had one of three cancers: lung, breast, or brain. The team also had access to a complete digital library of diagnostic CT and MRI images from the group, as well as medical records of patients’ treatment and outcome history.
In their study, Li and the team worked with medical professionals who begin by looking at and delineating the tumors in the scans. Based on knowledge of cancer biology, the team then engineered in key features, such as tumor growth patterns, and the diversity across different parts of the tumor, providing the AI a bit of a head start in its analysis. From there, a machine learning algorithm scoured the tumor image features for patterns.
Li’s algorithms were able to identify four tumor subtypes among the various cancers according to their distinct radiographical features. And, by knowing patients’ past treatment regimen and medical history, Li could then match these new subtypes to favorable treatments.
One lung cancer subtype identified in Li’s study, thought to be present in as many as half of advanced lung cancer patients, was shown to be associated with improved survival rates when treatment includes an immunotherapy known as “immune checkpoint blockade”—where drugs impede certain proteins known as checkpoints, which limit immune response, preventing the immune system from killing cancer cells. But with checkpoints removed—or blockaded—immune cells are made more effective.
“We believe this study represents a major scientific advance,” Li said. “It is the first radiological tumor classification system that is broadly applicable across imaging technologies and cancer histologies.”
Human-AI Collaboration
Li says the algorithm is able to spot patterns in a tumor’s radiographical features linked with the inner workings of the molecular biology that even trained medical professionals cannot. In fact, Li says, it is this collaboration between human knowledge and the computational power of AI that sets the research apart. It is not exactly the province of the traditional fields of radiology or oncology, but within a growing discipline known as radiomics.
“Radiomics is different from traditional deep learning in that it leverages the prior knowledge of human professionals in combination with the power of AI,” Li explained. “Radiomics requires human expertise as a key input to identify features. Then the machine learning predicts the outcome based on patient history.”
While Li’s research is promising, it is, as of now, a retrospective study on patients who have already been treated. However, it demonstrates the future feasibility of such AI approaches in clinical settings. Li imagines that his algorithm could soon be paired side by side with traditional oncological and radiological approaches in a proof-of-concept trial of AI’s ability to guide personalized treatment recommendations.
“Eventually,” Li said, “Deep learning could automate the process of tumor subtype identification and lead to potentially life-saving improvements in selecting treatment for patients.”
Stanford HAI's mission is to advance AI research, education, policy and practice to improve the human condition. Learn more.